
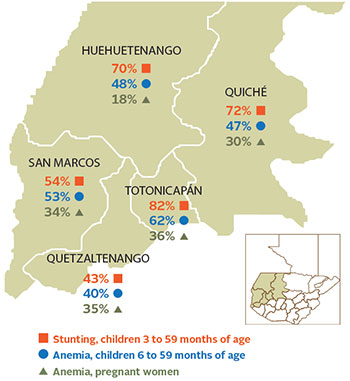
In the Western Highlands of Guatemala, where more than half of children under 5 are stunted, the Government of Guatemala’s 2012 Zero Hunger Pact aims to reduce the prevalence of stunting by 24% in 10 years. Stunting is attributable to poor complementary feeding practices, but also to poor maternal nutritional status during pregnancy. In addition to extremely high levels of stunting, micronutrient deficiencies (particularly irondeficiency anemia) affect approximately 20–35% of pregnant women. Anemia among children under 5 is also widely prevalent. Given that the first 1,000 days from pregnancy through a child’s second birthday is a critical period for preventing stunting, the Food and Nutrition Technical Assistance III Project (FANTA), funded by the U.S. Agency for International Development (USAID), worked to identify strategies using locally available foods to improve the nutritional quality of diets for children 6–23 months of age and pregnant and lactating women.
 In partnership with the Institute of Nutrition of Central America and Panama (INCAP), FANTA first used the Optifood tool to identify nutrient gaps in the diets of pregnant and lactating women and young children. Results determined that consuming adequate amounts of iron, zinc, calcium, and folate were likely to be difficult using local foods, particularly given existing diet patterns. Based on this information, FANTA identified a set of evidence-based and population-specific dietary recommendations, known as food-based recommendations (FBRs), designed specifically for young children and pregnant and lactating women. The FBRs took into account the nutritional requirements of the target population, nutrient content of locally available food, dietary preferences and patterns, and the cost of local foods. To help fill nutrient gaps, the FBRs included consumption of foods such as eggs, beans, vegetables, liver, and a fortified blended flour prepared as porridge for young children and thick atole drink for women.
In partnership with the Institute of Nutrition of Central America and Panama (INCAP), FANTA first used the Optifood tool to identify nutrient gaps in the diets of pregnant and lactating women and young children. Results determined that consuming adequate amounts of iron, zinc, calcium, and folate were likely to be difficult using local foods, particularly given existing diet patterns. Based on this information, FANTA identified a set of evidence-based and population-specific dietary recommendations, known as food-based recommendations (FBRs), designed specifically for young children and pregnant and lactating women. The FBRs took into account the nutritional requirements of the target population, nutrient content of locally available food, dietary preferences and patterns, and the cost of local foods. To help fill nutrient gaps, the FBRs included consumption of foods such as eggs, beans, vegetables, liver, and a fortified blended flour prepared as porridge for young children and thick atole drink for women.
FANTA then carried out household trials with families in Huehuetenango and Quiché to test the acceptability and feasibility of preparing and consuming the recommended foods with the specified quantity and frequency for young children, pregnant women, and lactating mothers. Qualitative methods such as semi-structured interviews, key informant interviews, focus group discussions, and observations of agriculture and livestock practices provided insights into important factors such as availability and access to foods, beliefs and preferences regarding children and women’s consumption of the foods, seasonality, agricultural practices, time available for women to engage in the recommended actions, and the existing enabling environment to support the implementation of the proposed FBRs.
Findings
The trial findings showed that the recommended foods were considered acceptable by the families who tried them, but with a strong preference for liquid preparations, such as bean broth instead of pureed beans, making these foods less nutrient dense. However, beliefs and preferences did not deter most women from trying the FBRs—mothers and pregnant and lactating women perceived them as a benefit to their own and their child’s well-being and felt motivated to try them. Despite this, putting the FBRs into practice with the recommended frequency and quantity was difficult. Challenges to implementing the FBRs included financial limitations of the family food budget, seasonal variation in home production and market prices, difficulties in accessing and storing fresh foods, and the cost and time associated with transport to markets.
Women found that the lack of physical and economic access to nutrient-dense food was an important barrier, demonstrating that improvements must come from strengthening access to nutritious food, as well as family support to select, purchase, prepare, and distribute the foods to pregnant and lactating women and young children in the household. The trials revealed a culture of sharing food equally among all family members and most trial participants said they would need to buy the recommended food for the whole family, thus increasing the cost. For the FBRs involving fortified blended flour, the government program that distributes the flour for pregnant and lactating women and young children was not active in the implementation area at the time of the trials. As a result, families could only practice these FBRs if they purchased a substitute product at a higher cost than the staple food.
Recognizing the difficulties that some families faced trying the FBRs, further Optifood testing was carried out to examine the impact of adjusting the FBRs to make their adoption more feasible, as well as combining the FBRs with different scenarios of micronutrient supplementation, multiple micronutrient powders, and fortified blended flour. The revised set of FBRs, which indicate foods to be consumed in addition to the regular diet, is shown in the figure below. While these foods fill most nutrient gaps, some gaps still remain and could be addressed through reformulation of micronutrient supplements or fortified products.

Implications and Recommendations
The findings show that it is possible to optimize and improve the quality of women and children’s diets by developing and promoting a set of FBRs based on an optimal set of nutrient-dense local foods that meet most nutrient needs. However, the results also indicate that in the communities in the Western Highlands of Guatemala where the trial was conducted, local foods as they are usually consumed are not enough to address the nutrient gaps and achieve diet adequacy. Other strategies, such as fortified foods or micronutrient supplements, are also needed. To improve the nutritional status of women and children and ensure a healthier, more productive future for Guatemalan children, it is crucial to address economic and market access, household food production, and optimal nutrition practices, as well as strengthen national programs (such as distribution of fortified foods and micronutrient supplements). Some of the recommendations from the trial include prioritizing the most nutrient-dense FBRs and promoting their economic access, supporting access to local markets or mobile vendors, ensuring the procurement and distribution of micronutrient supplements, and identifying and promoting other local foods with similar nutrient profiles for seasonal accommodations.
Next Steps
The results from the trial have provided valuable insights to help nutrition and food security programs identify alternative ways to improve women and children’s access to and consumption of highnutrient foods. For maximum impact, FBR findings should be integrated across USAID’s Western Highlands Integrated Program as harmonized strategies, key messages, and materials to assist the Government of Guatemala, USAID partners, and others to promote the adoption of the FBRs. For example, USAID/Guatemala and local implementing partners are organizing collaborative workshops to identify strategies to introduce or increase production of nutritious local foods such as black beans, green leafy vegetables, eggs, and chicken liver. Additionally, FANTA is helping identify strategies to improve family support to practice the FBRs in the home due to the important role that mothers-in-law and husbands/partners play in food purchase and preparation.
To support USAID and local partners in monitoring activities related to the implementation of the FBRs, a rapid monitoring tool is being developed to assess how the recommended foods are being promoted at the household and community levels, and to target improvements. FANTA is also working with INCAP to identify recommendations for reformulation of micronutrient supplements or fortified products to ensure that needed micronutrients complement the consumption of local foods. Finally, given Guatemala’s transition to a new government in early 2016, events are planned to share the FBR trial results and develop an action agenda with incoming government representatives from health, agriculture, and economic development sectors.


